Home > Revenue Cycle Management > Patient Access Solutions
Patient Access solutions
Improving patient experience with faster, easier access to care while protecting your revenue at every step
Patient financial clearance
Verify eligibility, validate registration, estimate liability, and secure prior authorizations automatically, so patients arrive cleared and claims go out clean.
MyCareHub: Patient engagement and schedule optimization
Built on a patient-first framework, MyCareHub uses behavioral intelligence to reduce confusion, personalize engagement, and guide patients through every step of their care journey, creating more informed patients, fewer no-shows, and better schedule utilization.
How our solutions work at every stage of the patient access journey
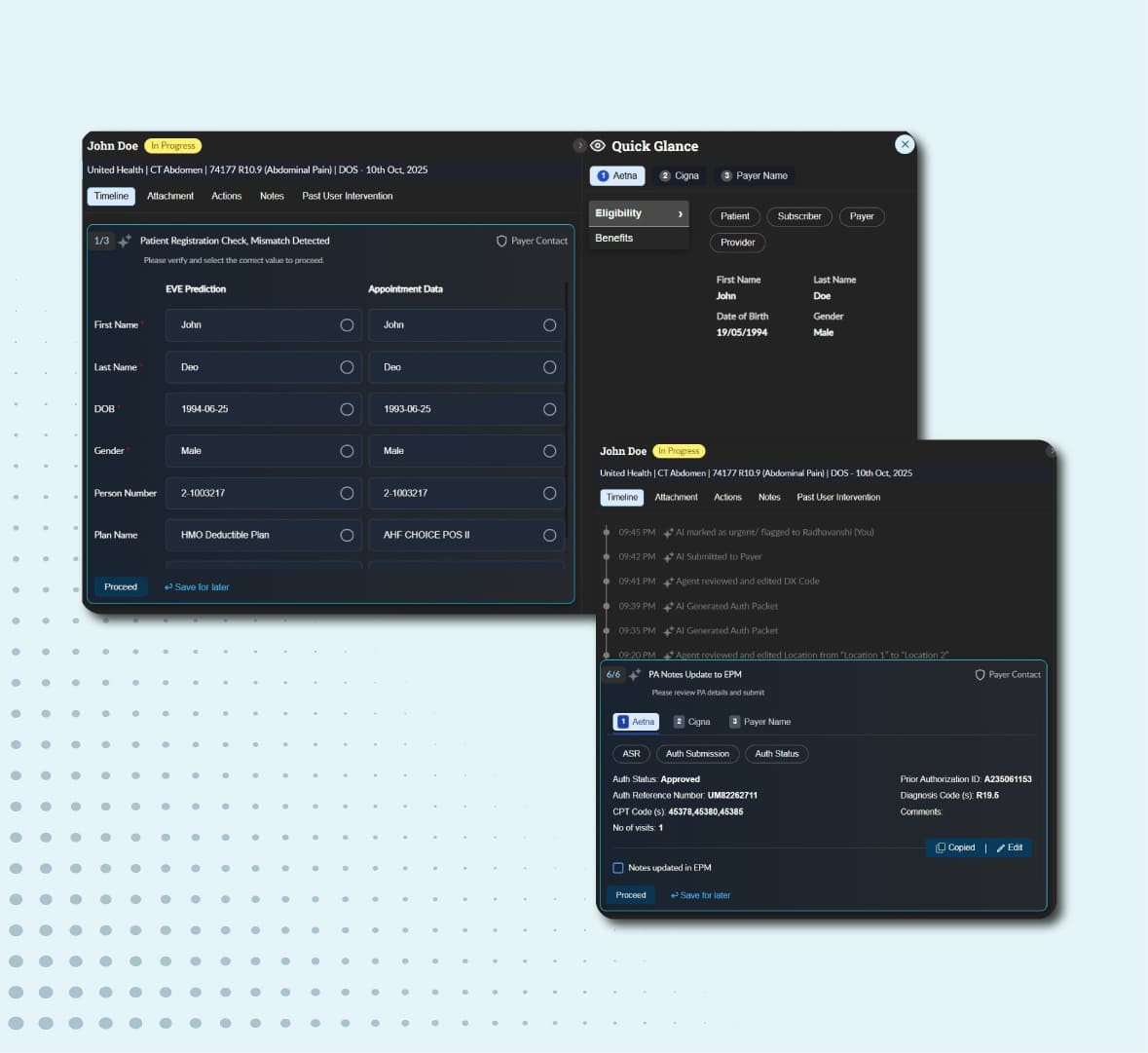
Patient financial clearance
IKS Health autonomously verifies eligibility, validates registration, estimates liability, and initiates authorizations before the patient walks through the door.
Real-time eligibility & benefits
Continuously verifies coverage and matches benefits to scheduled procedures, eliminating misalignments that lead to denials.
AI-driven registration integrity
Detects and corrects demographic errors using longitudinal patient profiles, preventing front-end denials before they occur.
Intelligent liability estimation
Produces accurate out-of-pocket estimates to drive pre-service collections and eliminate billing surprises.
Autonomous prior authorization
Agentic AI detects PA requirements from the IKS coding platform and EHR system, navigates payer portals, and submits forms in parallel. A human-in-the-loop model ensures expert teams resolve complex exceptions, while a full audit trail keeps every step compliance-ready.
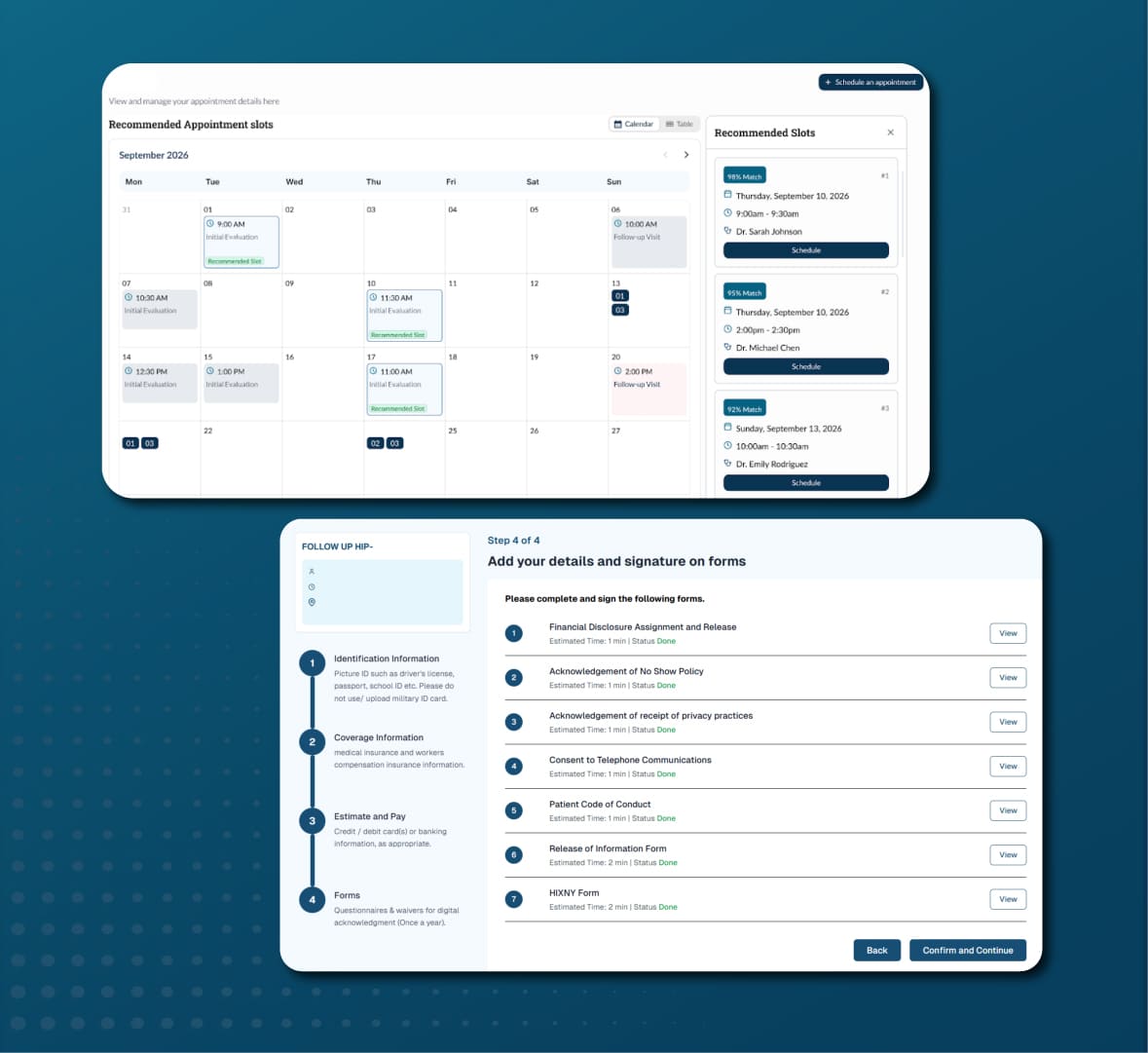
MyCareHub: Patient engagement and schedule optimization
A patient-first engagement platform that reduces patient burden through behavioral intelligence, driving readiness, adherence, and schedule efficiency as a natural outcome.
AAW behavioral profiling
Analyzes each patient’s awareness, ability, and willingness (AAW) to pay to predict payment and appointment adherence ,then automatically triggers the right action, from personalized reminders to flexible payment options or upfront collection.
Schedule optimization and recommendation
Replaces first-available scheduling with revenue-optimized slot placement using patient value, adherence, appointment performance, and payer settlement scores.
Self-service patient portal
Patients complete onboarding, verify identity, update coverage, and pay through a secure digital portal before their visit.
Behavior driven reminders and nudges
Appointment reminders, payment follow ups, and onboarding outreach optimized for timing, channel, and message style.
Driving key outcomes and results across healthcare organizations
95%
Patients cleared financially pre-visit
80%
Task automation for routine workflows
Reduced Denials With IKS EVE
A healthcare organization deployed IKS EVE with autonomous eligibility and benefits verification, achieving a denial reduction from $1M to $431K in just two quarters through registration integrity and payor knowledge-driven prior authorization.
Driving prior authorization excellence for a leading multi-specialty group
$2.4M cash upside in CY 2024. 99% case resolution without peer-to-peer escalation. Only 1 reschedule out of 99K requests processed.
“We are excited to expand our partnership with IKS Health as we pursue our goals of improving patient engagement within our practice. This partnership underscores our commitment to deliver exceptional patient experience.”
– CEO, OrthoNY
20-25%
Reduction in patient access costs
99.78%
Prior authorization processing accuracy rate
20%
Reduction in prior authorization denials
How our patient access solutions support patients
We make it easier for patients to start, navigate, and stay on track with their care, without the friction that usually gets in the way.
Faster access to care
Eligibility, authorizations, and registration handled before the visit, so patients aren't delayed by paperwork or insurance surprises.
Personalized experience
Outreach, reminders, and payment options tailored to each patient's preferences, behaviors, and financial situation.
Frictionless onboarding
Digital check-in, insurance capture with OCR, and payments completed in under a minute from any device.
Transparent costs
Accurate out-of-pocket estimates upfront, so patients know what to expect and can plan accordingly.
How our patient access solutions support healthcare organizations
By automating the manual work and surfacing the right information at the right time, we free your teams to focus on patients instead of paperwork.
Administrative relief
AI handles eligibility checks, registration validation, prior authorizations, and reminders. Staff only touch the exceptions.
Intelligent scheduling
No-shows predicted before they happen, cancellations auto-filled from a scored waitlist, and slots optimized for revenue yield.
Fewer denials, less rework
Errors caught and fixed at the front end, so billing teams aren't chasing down corrections weeks later.
Knowledge that stays
The system captures expert decisions and continuously learns, protecting your operations from staff turnover and tribal knowledge loss.
Ready to transform Patient Access?
Join leading healthcare organizations preventing uncompensated care, accelerating time-to-care, and maximizing revenue from every patient encounter.
Patient Access resources
Preactive Patient Access: Prevent Denials and Reduce Uncompensated Care in Healthcare
Breaking the Denial Cycle: The Future of Prior Authorization
Journey From Patient Outreach To Meaningful Patient Engagement: How Behavioral Economics May Help
Frequently Asked Questions
What is patient financial clearance?
Patient financial clearance verifies insurance eligibility, validates registration data, estimates patient liability, and confirms prior authorization requirements before a visit. IKS Health automates this entire workflow using AI that continuously learns across patient, payer, and provider dimensions.
How does autonomous prior authorization work?
IKS Health uses agentic AI to detect PA requirements from coded charts or EHR inputs, navigate payer portals, submit authorization forms, monitor status in real time, and resolve exceptions through human-in-the-loop triage. Up to 80% of routine PA workflows are processed automatically with 99.78% accuracy.
What is the AAW behavioral framework?
AAW is IKS Health’s proprietary, patent-pending model that evaluates patients on Awareness, Ability, and Willingness. It powers personalized engagement strategies, from outreach channel and tone to financial assistance options, maximizing both collections and appointment adherence.
How does schedule optimization improve revenue?
The schedule optimization and recommendation engine replaces first-available scheduling with revenue-optimized slot placement using patient value scoring, payer settlement indexing, and no-show prediction. This maximizes revenue yield per slot while reducing gaps through automated waitlist backfill.
Does IKS Health integrate with existing EHR systems?
Yes. The platform is EHR-interoperable via HL7 v2, FHIR, batch, and RPA. It works with existing EMR/PM systems with no disruption, deploys in weeks, and offers performance-based pricing.
What is MyCareHub?
MyCareHub is an agentic engagement platform that unifies onboarding, financial clearance, adherence, and schedule optimization. Powered by proprietary behavioral models , it predicts payment likelihood and appointment attendance to drive personalized, multi-channel outreach. Patient access teams work in a single environment where automated self-service workflows reduce no-shows, accelerate collections, and improve schedule yield, transforming the patient journey into a proactive, cognitive experience.



